How Do I Know If My Marijuana Use Is Too Much? Learning about Cannabis Use Disorder
If you’re reading this, you’re probably asking yourself a question that many marijuana users eventually face: “Has my use become too much?” Maybe someone close to you expressed concern. Maybe you’ve noticed changes — using more than you planned, feeling irritable when you can’t use, or struggling to cut back even though you want to.
These are important questions, and asking them is a sign of self-awareness, not weakness. Marijuana use exists on a spectrum — from occasional use with no problems to cannabis use disorder, a medical condition affecting approximately 1 in 5 regular users (Spiga et al., 2025). Cannabis use disorder is classified among addictive disorders, which also include other substance-related conditions such as alcohol and opioid use disorders. The challenge is that marijuana’s effects build gradually, so many people don’t realize their use has become problematic until it’s significantly affecting their health, relationships, or daily functioning.
This guide will help you honestly assess your marijuana use using the same criteria mental health professionals use to diagnose cannabis use disorder. You’ll learn the 11 warning signs, understand what makes use “too much,” and know when it’s time to consider getting help.
Understanding Cannabis Use Disorder
Cannabis use disorder (CUD) is a medical condition — not a moral failing. It’s defined by a pattern of marijuana use that causes real harm to your life, health, or relationships, and involves brain changes that make it difficult to stop using even when you want to. Problematic cannabis use is a form of drug abuse and represents a broader public health concern.
The numbers tell an important story: approximately 30% of past-year cannabis users meet criteria for cannabis use disorder (Kansagara et al., 2026). The risk varies dramatically based on frequency: while only about 3.5% of people who use marijuana yearly develop cannabis use disorder, that number jumps to 36% among daily or near-daily users (Gorelick, 2023). The risk of developing cannabis use disorder is approximately 9% among those who have consumed cannabis, which increases to 25% for daily users.
According to the 2019 National Survey on Drug Use and Health, 16.3 million people in the United States aged 12 years or older met the criteria for cannabis use disorder, representing 5.8% of individuals in that age range. This isn’t rare — it’s affecting millions, many of whom look successful and functional on the outside. Globally, an estimated 22.1 million people, or 0.3% of the world's population, were reported to have cannabis dependence. In the United States, cannabis is the most commonly identified illicit substance among individuals admitted to treatment facilities, with a significant portion referred by the criminal justice system.
The 11 Warning Signs of Cannabis Use Disorder
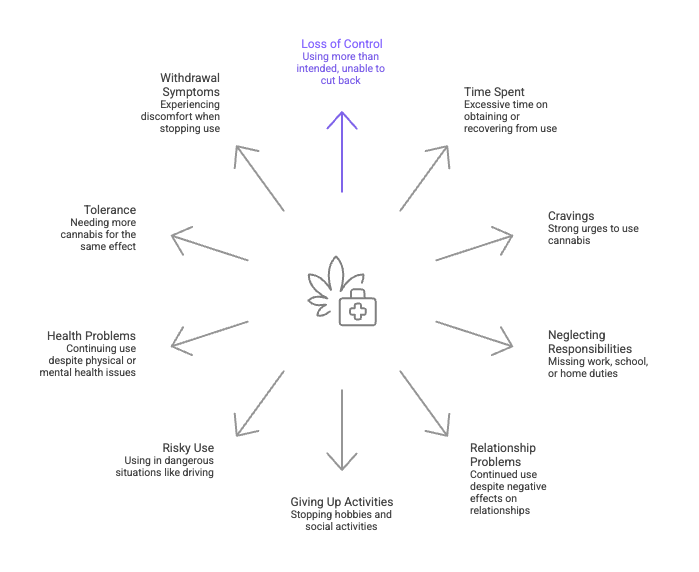
Mental health professionals use 11 specific criteria from the Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR) to diagnose cannabis use disorder (American Psychiatric Association, 2022). If you recognize 2 or more of these in yourself over the past 12 months, your marijuana use may have crossed into problematic territory (also referred to as problematic cannabis use).
Loss of Control Over Use
1. Using more than you planned
You intended to have just a little, but ended up using more — or using for longer — than you meant to. You tell yourself you'll only smoke on weekends, but by Wednesday you're using again.
2. Wanting to cut back but not being able to
You've tried to reduce or stop your marijuana use, but haven't been successful. You keep telling yourself you'll cut back "tomorrow," but tomorrow never comes. Individuals with cannabis use disorder may find it difficult to stop using cannabis even when they want to, indicating a loss of control.
3. Spending a lot of time on marijuana
A significant portion of your day revolves around getting marijuana, using it, or recovering from its effects. Approximately 1 in 3 medical cannabis patients in Maryland meet the criteria for cannabis use disorder, often indicated by excessive time spent obtaining or recovering from use.
4. Experiencing cravings
You experience a strong desire or urge to use marijuana, especially in certain situations or at certain times of day. Common symptoms of cannabis use disorder include cravings for cannabis, which can be triggered by stress, certain places, or specific times.
Impact on Your Life
5. Falling behind on responsibilities
Your marijuana use is causing you to miss work, perform poorly at school, or neglect responsibilities at home. Social or occupational impairment refers to neglecting responsibilities at work, school, or home due to cannabis use. These issues are part of broader cannabis related problems, which can include health, social, and functional impairments resulting from problematic cannabis consumption. In Baltimore’s competitive professional environment, this might show up as decreased productivity or missing important meetings.
6. Continued use despite relationship problems
You keep using even though it’s causing arguments with your partner, family, or friends. An important marker of severe cannabis use disorder is continued use despite negative effects on important relationships (DSM-5-TR).
7. Giving up activities you used to enjoy
You’ve stopped or reduced participation in hobbies, social activities, or other things that used to matter to you because of marijuana use. Activities that don’t involve marijuana just seem less interesting.
Risky Use
8. Using in dangerous situations
You use marijuana before driving, operating machinery, or in other situations requiring alertness and coordination. Risky use includes continued cannabis consumption in dangerous situations. Cannabis use has been linked to an increased risk of motor vehicle accidents, contributing to traffic-related injuries and fatalities. In Maryland, there has been a nearly 44% rise in cannabis-related emergency department visits among young adults (ages 20–29) between 2022 and 2023.
9. Continuing despite health problems
You keep using even though you know marijuana is causing or worsening a physical or mental health problem. Chronic cannabis use can lead to physical health complications such as chronic cough and respiratory issues, as well as mental health issues like increased anxiety and depression.
Physical Dependence
10. Tolerance
You need more marijuana to get the same effect you used to get with less, or the same amount doesn’t work as well. Tolerance develops as your brain adapts to regular cannabis exposure, due to reduced availability of cannabinoid receptors (Page et al., 2020). Chronic administration of cannabis leads to neurobiological changes that underlie both tolerance and dependence.
11. Withdrawal symptoms
When you stop or significantly cut back, you experience uncomfortable symptoms. Cannabis withdrawal is real and more common than most people realize. Withdrawal occurs in almost 50% of daily users (Gorelick, 2023). Heavy cannabis use can lead to withdrawal symptoms such as irritability, insomnia, and decreased appetite.
In our work with clients at the Baltimore Therapy Group, we see how hard it is to recognize when marijuana use has crossed the line — especially in a culture where cannabis is legal and widely accepted. Many people come in saying “I didn’t think I had a problem because I’m not using hard drugs.” But cannabis use disorder is real. The 11 criteria aren’t arbitrary — they describe patterns we see every day: talented professionals whose careers are stalling, relationships eroding, or mental health deteriorating. Recognizing the pattern is the first step.
How Cannabis Withdrawal Actually Feels
Many people are surprised to learn that marijuana causes genuine withdrawal symptoms. Withdrawal syndrome has a prevalence of 17% among regular users overall, and nearly half of daily users experience it (Hsu et al., 2025).
The typical timeline (Gorelick, 2023; Connor et al., 2022):
Begins: Within 1-2 days after stopping
Peaks: Within 2-6 days
Lasts: 1-3 weeks (though sleep problems may persist longer)
Common withdrawal symptoms include irritability, anger, anxiety, difficulty sleeping, vivid dreams, decreased appetite, restlessness, depressed mood, cognitive impairment, and physical symptoms like headaches, sweating, chills, or stomach pain.
Withdrawal is not dangerous, but it is uncomfortable — and it’s one of the main reasons people who want to quit end up using again. Withdrawal severity tends to be greater in those with problematic cannabis use. Some people mistake withdrawal symptoms for underlying mental health problems, leading them to continue using marijuana to “treat” what is actually a withdrawal effect.
Assessing Severity: Mild, Moderate, or Severe?
The number of warning signs you experience indicates severity (DSM-5-TR):
2-3 signs = Mild cannabis use disorder
4-5 signs = Moderate cannabis use disorder
6 or more signs = Severe cannabis use disorder
About half of people diagnosed with cannabis use disorder have moderate to severe disease, meaning it contributes significantly to negative social, employment, or other life impacts (Kansagara et al., 2026).
Red Flags Beyond the Clinical Criteria
Beyond the formal DSM-5 criteria, everyday signs that your marijuana use may be too much include:
Using marijuana more often or in larger amounts than you intended
Spending a lot of time getting, using, or recovering from marijuana
Craving marijuana or feeling unable to cut down
Neglecting responsibilities at work, school, or home due to marijuana use
Continuing to use marijuana despite social or relationship problems it causes
It's important to note that certain factors, such as starting marijuana use at a younger age, using more frequently, or having a family history of substance use disorders, can increase the risk of developing cannabis use disorder (CUD). Marijuana is one of many psychoactive substances that can lead to dependence and addiction, affecting the brain's reward system and potentially resulting in behavioral and biological changes.
Your Daily Routine Revolves Around Marijuana
You use first thing in the morning or throughout the day, and using cannabis daily is associated with a higher risk of developing cannabis use disorder (CUD)
You feel like you can’t relax, eat, sleep, or socialize without it
You plan your schedule around when you can use
You spend significant money on marijuana that could go toward other needs
Your Mental Health Is Suffering
You feel more anxious or depressed than before you started using regularly
You’re using marijuana to cope with stress, sadness, or anxiety rather than for enjoyment
You feel foggy, unmotivated, or “flat” much of the time
You’ve noticed memory problems or difficulty concentrating
Individuals diagnosed with cannabis use disorder often use cannabis as a form of self-medication to manage symptoms of existing mental health conditions. Cannabis use disorder frequently co-occurs with other psychiatric comorbidities, including major depressive disorder, bipolar disorder, and various anxiety disorders, as well as other substance use disorders such as alcohol or nicotine dependence.
The paradox: while people often start using marijuana to manage anxiety or depression, regular cannabis use is associated with increased risk of depression, anxiety, and psychotic symptoms, especially with high-potency products containing ≥10% THC (Hsu et al., 2025).
Your Relationships Are Affected
People close to you have expressed concern about your use
You hide how much you use from others
You prefer using alone over spending time with friends or family
You've lost friendships or had relationship conflicts because of marijuana
You feel defensive when anyone questions your use
Your Performance Has Declined
Your work or school performance has dropped
You've been late, absent, or less productive because of marijuana use
You've lost motivation for goals that used to be important to you
In Baltimore's high-achieving professional culture, you might maintain the outward appearance of functioning while internally struggling. High-functioning cannabis use disorder is real: you can hold down a job, maintain relationships on the surface, and still meet criteria for a substance use disorder.
You've Noticed Physical Changes
Chronic cough, wheezing, or breathing problems (if you smoke)
Recurring nausea, vomiting, or abdominal pain — about 2% of surveyed cannabis users in Maryland report experiencing Cannabis Hyperemesis Syndrome, characterized by severe, recurrent vomiting. It affects 32.9% of patients who smoke cannabis ≥20 days/month (Hsu et al., 2025)
Weight changes
Increased heart rate or cardiovascular symptoms
Who Is Most at Risk for Cannabis Use Disorder?
Some people are at higher risk for developing problematic marijuana use and marijuana addiction:
Frequency of use: The major risk factors for cannabis use disorder are frequency and duration of use (Gorelick, 2023). Daily cannabis use significantly increases the risk, with studies showing an 8-fold increase in risk for daily users compared to those who use cannabis yearly. Strategies for lower risk cannabis use include avoiding high-potency products, limiting frequency of use, and choosing safer consumption methods to reduce the likelihood of developing CUD.
Starting young: A younger age of initiation of cannabis use is associated with a faster progression to cannabis use disorder, with the median age of onset being 22 years. Beginning marijuana use as a teenager significantly increases risk and may affect brain development, increasing the chance of developing CUD.
Higher potency products: The THC content has more than doubled over the past two decades — from about 3% in the 1980s to 17% in 2017 — and concentrates can exceed 90% THC (Spiga et al., 2025). High-potency cannabis (≥10% THC) is associated with higher rates of psychotic-like experiences** (12.4% vs. 7.1%) and generalized anxiety disorder (19.1% vs. 11.6%)** compared to lower-potency products (Hsu et al., 2025).
Mental health conditions: Having depression, anxiety, PTSD, or other psychiatric disorders increases vulnerability. For many people in Baltimore, seeking specialized anxiety therapy with evidence-based treatment options can be an important part of reducing reliance on cannabis. About half of people who experience a mental health condition will also experience a substance use disorder and vice versa, a phenomenon known as dual diagnosis.
Family history: Genetic factors account for 40% to 60% of the vulnerability to cannabis use disorder, with individuals having a first-degree relative with a substance use disorder being at higher risk. A history of trauma in the family can also increase vulnerability, and many people benefit from trauma-focused therapy in Baltimore to address underlying wounds that contribute to substance use.
Other substance use: Using alcohol, tobacco, or other drugs alongside marijuana increases risk.
The prevalence of cannabis use among Australians aged 14 years and over is reported at 34.8%, indicating a significant level of use in this demographic.
A Quick Self-Assessment
Ask yourself these questions honestly (based on the 11 DSM-5 criteria):
Have I ever used marijuana for longer or in larger amounts than I intended?
Have I tried to cut back or stop and been unable to?
Do I spend a lot of time getting, using, or recovering from marijuana?
Do I crave marijuana?
Has my marijuana use caused problems at work, school, or home?
Do I continue to use despite problems it causes in my relationships?
Have I given up activities I used to enjoy because of marijuana?
Have I used marijuana in situations where it was physically dangerous?
Do I continue to use even though I know it's causing or worsening a health problem?
Do I need more marijuana to get the same effect?
Do I feel withdrawal symptoms when I stop?
If you answered "yes" to 2 or more of these questions, your marijuana use warrants a closer look. This doesn't necessarily mean you need to stop completely — but it does mean your use has crossed into territory where it's causing problems.
You can also use validated screening tools like the Cannabis Use Disorder Identification Test-Revised (CUDIT-R), which showed good accuracy in distinguishing between adults with and without cannabis use disorder, with a cut-point of 9 yielding 87.8% sensitivity (Coelho et al., 2024).
The Mental Health Connection
Marijuana and mental health have a complicated, bidirectional relationship:
Cannabis can worsen mental health conditions. While many people use marijuana to cope with anxiety or depression, regular use can actually make these conditions worse over time. This creates a cycle: you feel bad → you use marijuana to feel better → marijuana worsens your mental health → you feel worse → you use more marijuana. Marijuana use can also sometimes progress to broader substance abuse, especially among youth, raising additional risks and concerns.
Heavy cannabis use in young people is linked to a higher risk of developing subsequent schizophrenia or psychosis according to research from Johns Hopkins Public Health.
It can be hard to tell what’s causing what. If you’re using marijuana regularly and experiencing anxiety, depression, or other mental health symptoms, it can be difficult to know whether marijuana is causing the symptoms, making them worse, or whether you’re using because of pre-existing symptoms.
A period of abstinence (at least 2-4 weeks) can help clarify this. The good news: neurocognitive deficits and cognitive impairment from cannabis use in adults may be reversible after approximately 25 days of abstinence (Hsu et al., 2025). Learning and memory impairments are consistently associated with heavy use but appear to recover after a period of abstinence (Kroon et al., 2020).
We often tell clients: if you’re using marijuana daily for anxiety or depression, you’re conducting an uncontrolled experiment on your brain. The only way to know if cannabis is helping or hurting is to stop for a few weeks and see what happens. Many people are shocked to discover that the anxiety they’ve been “treating” with weed actually gets better after the withdrawal period ends. The marijuana was the problem, not the solution. That clarity — understanding what you’re actually dealing with — is invaluable.
What You Can Do If You're Concerned
Talk to a Professional
Your healthcare provider or therapist can screen for cannabis use disorder in a confidential, nonjudgmental way and help you understand your options. The Single Item Screen-Cannabis has high negative predictive value for ruling out cannabis use disorder, while positive screens should be followed by the 8-item CUDIT-R (Kansagara et al., 2026).
In Baltimore, you can reach out to therapists who specialize in substance use at the Baltimore Therapy Group for expert counseling and support. We serve clients throughout Towson, Roland Park, Canton, Fells Point, Mt. Washington, and surrounding areas.
Consider a "Marijuana Check-Up"
A "marijuana check-up" is a brief (1-2 session) assessment where a counselor helps you look at your use patterns, weigh the pros and cons, and decide if you want to make changes. Even 2-session interventions produced significant reductions in frequency and daily duration of cannabis use at all follow-ups over 12 months (Stephens et al., 2021).
Try a Period of Abstinence
Taking a break for 2-4 weeks can help you see how you feel without marijuana, determine whether symptoms you attributed to other causes are actually related to marijuana, assess whether you can stop comfortably, and allow cognitive effects to reverse.
Explore Evidence-Based Treatment Options
If you decide you want help reducing or stopping your marijuana use, effective treatments are available. For parents, it can also be important to consider how your use and your child’s mental health interact, and some families choose to seek specialized child therapy in Baltimore for emotional and behavioral concerns:
Cognitive Behavioral Therapy (CBT): Helps you identify and manage the thoughts, behaviors, and triggers that lead to marijuana use. Our practice offers Cognitive Behavioral Therapy (CBT) with experienced therapists in Baltimore. Many clients also benefit from psychodynamic psychotherapy to explore underlying patterns driving their substance use. Psychological interventions, including motivational enhancement therapy and cognitive behavioral therapy, are currently the primary treatment options for cannabis use disorder (Gates et al., 2016).
Motivational Enhancement Therapy (MET): A collaborative, goal-oriented style of communication that aims to strengthen personal motivation for change** by exploring reasons for change and resolving ambivalence** (Schwenker et al., 2023). MET typically involves 1-4 sessions of about an hour each.
Combination approaches: Combination treatments that integrate motivational enhancement therapy and cognitive behavioral therapy have been shown to improve outcomes, including reduced frequency of use and increased abstinence rates.
Self-directed approaches: Participants receiving a CBT/MI-based self-directed workbook plus a single MI session showed greater reductions in frequency of use and higher rates of abstinence at 3 months compared to workbook alone (Schluter et al., 2022). Some people prefer to work with specific clinicians who focus on addiction and related concerns, such as the other practitioners at Baltimore Therapy Group who specialize in anxiety, trauma, and addiction.
Important to know: No pharmacological interventions have been approved for the treatment of cannabis use disorder. Treatment is primarily through counseling and behavioral approaches.
One thing we emphasize: seeking help for cannabis use disorder doesn't mean you've failed or that you're weak. It means you're paying attention to the impact marijuana is having on your life. We've worked with high-functioning people who never imagined they'd need help with marijuana.
Support Groups and Family Support
Support groups such as Narcotics Anonymous, Marijuana Anonymous, and online group therapy for anxiety and related concerns provide accountability and community for individuals in recovery. Peer support can be particularly valuable for people who feel isolated, and some couples also find that couples therapy and marriage counseling in Baltimore helps them repair relationship strain caused by cannabis use.
Family therapy and education** can improve communication within families, creating a supportive environment essential for recovery.**
Harm Reduction: If You're Not Ready to Stop
If you’re not ready to quit completely, you can still reduce your risk:
Decrease cannabis use as a harm reduction strategy. Gradually decreasing cannabis can help lower addiction severity and related health risks.
Use less frequently. Even reducing from daily to weekly use significantly lowers your risk
Avoid high-potency products. Lower-THC products carry less risk for psychosis, anxiety, and dependence
Don’t smoke. Edibles or vaporizers may reduce respiratory harm (though they carry their own risks)
Don’t drive after using. Marijuana impairs coordination, reaction time, and judgment
Avoid using to cope with emotions. Using marijuana as your primary way to manage stress increases dependence risk
Take regular breaks. Periodic abstinence can help prevent tolerance and dependence
Avoid mixing with alcohol or other substances. Combining substances increases risks
When to Get Help Right Away
Seek immediate help if you experience:
Thoughts of suicide or self-harm
Severe anxiety or panic that won't go away
Psychotic symptoms (hearing or seeing things that aren't there, paranoid thoughts)
Uncontrollable vomiting (Cannabis Hyperemesis Syndrome)
Chest pain or cardiovascular symptoms
SAMHSA National Helpline: 1-800-662-4357 (free, confidential, 24/7)
988 Suicide and Crisis Lifeline: 988
Baltimore County Crisis Response System: 410-931-2214 (24/7)
Finding Support in Baltimore
If you're concerned about your marijuana use and live in the Baltimore area, you don't have to figure this out alone. At the Baltimore Therapy Group, our experienced therapists understand cannabis use disorder and can provide evidence-based treatment including CBT, motivational enhancement therapy, and support for co-occurring mental health conditions. You can schedule therapy with a Baltimore therapist online or in person. We serve clients throughout Baltimore, Towson, Roland Park, Canton, Fells Point, Mt. Washington, and surrounding areas.
We can help you:
Assess whether your marijuana use has become problematic
Understand the relationship between your cannabis use and mental health
Develop a personalized plan for reducing or stopping use with the Baltimore Therapy Group, which is currently accepting new patients
Build healthier coping strategies for stress and emotions
Address underlying anxiety and depression through individual therapy or trauma, and explore whether symptoms like inattention, restlessness, or impulsivity might be related to ADHD and benefit from specialized ADHD therapy in Baltimore
Navigate relationships affected by your marijuana use
Maintain changes and prevent relapse
Cannabis use disorder is a real, treatable medical condition — not a moral failing. Many people also struggle with depression alongside cannabis use, and specialized depression therapy in Baltimore can be an important part of recovery. Most people who seek treatment experience meaningful improvement. The key question isn't whether marijuana is "good" or "bad," but whether your personal use is causing harm to your health, relationships, work, or overall quality of life.
If you recognize warning signs in yourself, effective help is available, including flexible teletherapy with online therapists in Baltimore. While less than 50% of patients sustain long-term abstinence (Gorelick, 2023), many significantly reduce their use and improve their quality of life. The hardest step is often the first one: being honest with yourself about whether your use has become too much.
Schedule an appointment with the Baltimore Therapy Group today.
Disclaimer: This article is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or qualified mental health provider with any questions you may have regarding a medical or mental health condition. If you are in crisis or experiencing thoughts of self-harm, please call 988 (Suicide and Crisis Lifeline) or go to your nearest emergency room.